
Canine melanoma: when sunscreen won’t help
Canine malignant melanoma is a highly metastatic disease where up to 80% of dogs with the disease will develop metastases. Melanomas are either benign or malignant tumours of melanocytes. Tumours of melanocytic origin are the most common malignancies of the oral cavity, skin, and eyes in dogs. The oral cavity is the fourth most common site of cancer in dogs. Malignant melanoma is the most common canine oral neoplasm and has a fair to poor prognosis. In dogs, more than 90% of oral melanomas are malignant, while 50% or less of cutaneous melanomas and 18% of intraocular melanomas are malignant.
Oral melanomas are locally invasive, and bone involvement is not uncommon. Metastasis to the local or regional lymph nodes or lungs is common although patients can present with widespread metastasis. Although digital (nail bed) melanomas are rare, they have a high metastatic rate. Affected dogs often have pulmonary micro-metastasis before diagnosis. Melanomas are also the most common canine intraocular tumours.
Oral melanoma (Figure 1)
• Common in poodles, Scottish terriers, dachshunds, and golden retrievers
• More common in older dogs (mean age 8-12 years)
• Clinical signs include a bleeding oral mass, loose teeth, persistent halitosis, dysphagia
• Characterized by rapid growth, local invasiveness, metastasize early
• Masses are often pigmented; amelanotic (no pigment) are also common
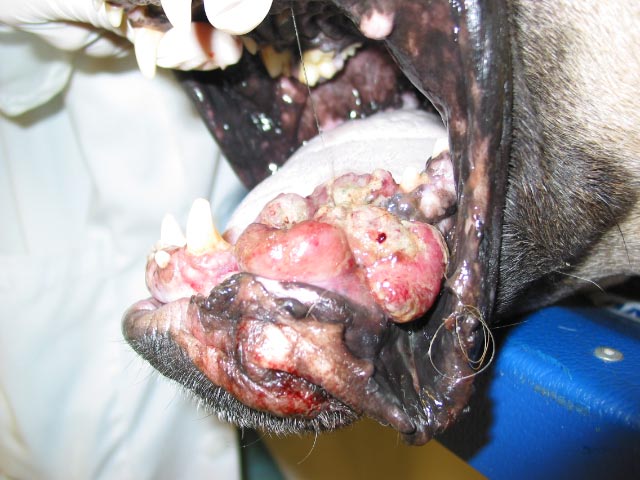
Figure 1. Oral melanoma
Cutaneous melanoma
• Airedales, Boston terriers, cocker spaniels and Scotties are predisposed
• Older (mean age 9 years) dogs with no sex predilection
• Can be benign or malignant and occur anywhere on body
• Common sites are the face (eyelids), trunk, and extremities
Melanoma of the digit (subungual melanoma)
• Highly malignant, especially in large black dogs
• Broken toe nail, mass on skin around digit; may be ulcerated
Ocular melanona
• Middle aged (6-7 years), medium to large breed dogs are predisposed
• Clinical signs include a visible intraocular mass, ruptured cornea, hyphema, glaucoma, and anterior uveitis
• Limbal and choroidal melanomas are benign tumours that have not been reported to metastasize after enucleation
• Anterior uveal melanoma is the most common primary intraocular tumour in dogs
• May also arise from the iris and ciliary body or choroid
Diagnostics and clinical staging
• Perform physical and oral examinations
• Measure mass and aspirate if feasible
• Palpate the regional lymph nodes and aspirate even if palpably normal
• Perform a surgical biopsy in patients with suspicious fine needle aspirates. Biopsy is gold standard for diagnosis
• Note: It can be difficult to diagnose a melanoma if the cells are poorly differentiated or amelanotic. Melanomas can be misdiagnosed as round-cell tumours, epithelial tumours, or anaplastic sarcomas. Immunohistochemistry could be helpful in confirming a diagnosis of melanoma although it is not infallible
• Minimum data base (CBC, chemistry panel, urinalysis)
• Thoracic radiographs – evaluate for metastatic disease
• With or without abdominal ultrasound – metastatic disease possible to liver and regional lymph nodes
• With or without skull radiographs or CT to determine the extent of local invasion into the nasal cavity, caudal pharynx, and orbit
Prognostic factors
Less information is available to determine the prognosis for dogs with melanoma than for people. One of the major prognostic factors includes size of the tumor. Masses that are smaller than 2cm in the oral cavity have a more favorable prognosis. In addition, masses located in the rostral mandible have a more favorable prognosis because of the greater likelihood of removing all of the disease. However, because the metastatic rate is high regardless of these factors, even if the tumour does not re-occur, metastasis will occur.
With regard to oral/lip melanomas and cutaneous/digit melanomas, a recent paper (Vet Path 2011) made recommendations for prognostication. After a literature review, the researchers determined that advanced stage of disease (distant metastasis, lymphatic metastasis) carried a poor prognosis. Other factors recommended to help determine a prognosis were mitotic rate, nuclear atypia, degree of pigmentation, presence of ulceration, level of invasion, and proliferation rate (using markers such as Ki67).
Treatment
There is no single completely effective treatment for advanced melanoma in dogs. Early detection and prompt initiation of treatment control tumour progression to a large extent. The choice of therapy is influenced by tumour type, location, extent of involvement, and the animal’s physical condition. Treatment modalities for canine melanoma include radical surgical resection, radiation therapy, chemotherapy, immunotherapy, and immunotherapy.
Surgery
The treatment for dogs with melanoma without distant metastatic disease on staging starts with local tumour control. This is generally best completed through surgical removal of the mass due to its speed, increased curative intent, and reduced cost compared with other modalities. The extent of surgery is generally based on the anatomic site and size of the melanoma, with cutaneous melanomas usually requiring lumpectomy and all other sites requiring more aggressive and wide excision. While large resections such as partial mandibulectomy or maxillectomy carry an inherent level of morbidity, owner satisfaction rates are routinely considered high.
Radiation therapy
Radiation therapy plays a role in the treatment of canine melanoma when the tumour is not surgically resectable, the tumour has been removed with incomplete margins, and/or the melanoma has metastasized to local lymph nodes without further distant metastasis.
Chemotherapy
In general, it appears, as in people, that canine melanoma is an extremely chemotherapy-resistant tumour. However, chemotherapy has been used in an adjuvant setting and modest responses have been seen. One study reported an overall response rate of 28% using carboplatin for dogs with malignant melanoma. Similarly, another study reported an 18% response rate and median survival time of 119 days with cisplatin and piroxicam in canine oral melanoma.
Immunotherapy
The melanoma vaccine

Figure 2. Melanoma vaccine injection
Merial launched Oncept in 2006. Conventional vaccines (for other common diseases) stimulate an immune response directed against foreign proteins. Tyrosinase, a protein present on canine melanoma cells, is not usually targeted by the dog’s immune system because it also is present on normal canine cells. Oncept trains the immune system to recognize this cancer-associated protein as a threat to the dog’s health. The vaccine is produced with a non-canine gene for tyrosinase inserted in a small ring of DNA. This foreign tyrosinase is different enough from canine tyrosinase to break through the dog’s tolerance of a self-tumour, so it induces a strong and active immune response. The vaccine is given by injection with a special device (see Figure 2) every two weeks for a total of four treatments and then once every six months thereafter. There are minimal to no side effects.CVT




